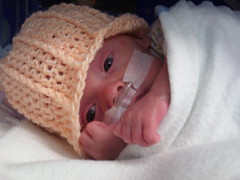
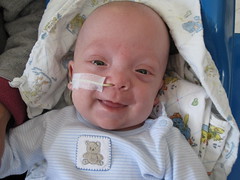
We had a "family meeting" today; our first in two months. Max's entire NICU team assembled in a conference room adjacent to the critical care nursery: the attending, fellow, resident, Max's nurse and a social worker, plus maybe a couple other cast members took two hours out of their day to talk to us and answer our questions. I feel like writing a personal note of apology to all of the babies in the NICU because we sucked up so much of the NICU team's collective brainpower.
We learnt quite a bit: too much for me to detail tonight. I will hit the high points now and then write a longer description later. (If you stick around to the end of this post you'll be rewarded with a heart-warming story.) The attending began the discussion of each of Max's problems by asking us to describe our perception of the situation. The picture that Carolyn and I described seemed to accord well with the NICU team's in almost all cases, so there weren't (many) surprises.
I'll start with Max's head because I believe that, although it is not an urgent problem right now, many years from now we'll still be dealing with Max's hydrocephalus long after we've forgotten about his reflux or breathing problems. Thus, any kind of news about his hydrocephalus affects my vision of life in the science-fictional year of 2030 (when I hope to attend Max's college graduation). As we knew, Max has hydrocephalus, but his most recent MRI showed no sign of PVL. However, Dr. S. said that in addition to being swollen (the hallmark of hydrocephalus), Max's left ventricle was oddly shaped. I think that Dr. S. adduced that the ventricle may have flowed into an area of "lost brain". As I understand it, until now we'd been worried about the damage that Max's ventricles did to the surrounding brain tissue when they filled with CSF and expanded. However, Dr. S. seemed to suggest that, like a water balloon sitting on some Legos, one of Max's ventricles might be larger than normal because there was no brain tissue there to push back. This was all very confusing, and we asked several questions about it but couldn't quite nail down what had happened. Carolyn and I have decided to suspend our anxiety on this matter and consult with a neurologist next week. We also learnt that 20 percent of infants with enlarged ventricles go on to have some kind of motor or cognitive deficit.
We can't control what's going on inside Max's brain. However, I'm firmly convinced that aggressive therapy can ameliorate any damage. Dr. S. and the NICU team clearly relaxed when we said that we intended to sign Max up for the local early intervention program and follow the advice of speech/physical/occupational therapists. Years of graduate school have prepared Carolyn and me to compulsively follow any therapeutic regimen suggested by the experts. I also told the NICU team what they couldn't know: that Max's older brother is as sharp as a tack, and that his parents aren't dullards either. Hence, Max himself must be in line to inherit some grade A brains. This was the one comment I made that elicited hearty laughter from the whole NICU team. Perhaps Max's dad isn't as smart as he thought.
The NICU team told us that a recent assessment of Max's reflexes, behavior, etc put him at the same level as a normal baby aged one month. (Max is more than three months old.) I think the NICU team were afraid that this would dismay us, but Carolyn and I were thrilled by the news. Considering that for weeks and weeks of his early tenure at the NICU, Max wasn't even as responsive as a normal newborn infant, this is a huge step forward.
Dr. S. was quite upbeat about the state of Max's lungs. First, the bad news: the lungs were damaged by the use of oxygen therapy and respirators in his early weeks at the NICU, plus the normal underdevelopment of the lung of the premature infant. In addition, Max is aspirating his reflux (see below) further damaging them. The inflammation from inhaling liquids is what is causing his persistent pulmonary edema, which decreases the efficiency of his lungs.
Now the good news. The lung seems to be the one organ that NICU teams really love. It grows relatively quickly in relation to the infant's overall growth, and grows for a long time. By the time Max is two years old, the damaged portion of his lung will represent only a small fraction of his overall lung. Even if Max's reflux continues to damage his lung, it will grow its way out of trouble. The danger to Max's lung is that he aspirates a considerable quantity of milk and develops pneumonia: this could affect a significant fraction of his lung.
Finally, we spent quite a lot of time talking about Max's main problem: his reflux. Really, his reflux is the main reason Max is still in the hospital. I think they would have sent him home with a feeding tube by now. But when Max is fed he is very uncomfortable and is clearly feeling his stomach contents travelling up his esophagus. He vomits much more frequently now than ever before in his stay at the NICU. To Carolyn and me this reflux seemed to come out of nowhere. However, the NICU team told us that they've increased the volume that Max is getting. This is actually good news: despite his reflux and vomiting, Max is managing to get enough nutrition from his feeds that he is gaining weight. Indeed, in a very narrow sense, I believe that Max is actually maybe thriving. Some babies require supplemental nutrition via an IV. In addition, back during the dark days of mid-December, I remember Max's nurses describing his symptoms as consistent with reflux. Shortly after that, the NICU team pushed his feeding tube into his duodenum, where it was more or less impossible for milk to return to the stomach and then reflux back to the esophagus.
The NICU team are urging us to seriously consider a couple of linked surgical procedures. First is running a tube--called a g-tube--to Max's stomach directly from the outside world. This will allow us to feed him without using a feeding tube. If Max didn't have reflux but was just having trouble eating, a g-tube would allow us to take him home immediately. The second is called the Nissen procedure and involves, effectively, tightening the esophagus's opening into the stomach. This surgery elicits a lot of controversy on the Internet. Many parents seem to feel that their doctors suggest it as a way to get a baby to stop screaming in discomfort from reflux, but that the procedure itself doesn't actually do much. In adults, the procedure isn't that successful.
The good news is that the NICU team are very conservative and will consult closely with the pediatric surgeon. They're ordering a couple of barium studies of his esophagus to see whether there's a structural abnormality that might make Max a good candidate for a Nissen. We've gotten to know the surgeon quite well over the past few months because Max has come close to requiring his services at least twice. We like and trust him. He wasn't the least bit disappointed in the past episodes when Max got himself organized and avoided the surgeon's knife.
And now, the heart-warming story. Carolyn went out for coffee with a colleague this afternoon. When she returned, she found that Max's nurses had rigged up a system of pads to allow him to be slightly propped up but also comfortable. She had also set up a toy star with a little mirror on it just within Max's reach. Carolyn found Max happily reaching up and batting at the star. From her description, it seems like Carolyn spent some time just staring at the scene: a baby playing happily with a crib toy.
Showing posts with label headbleed. Show all posts
Showing posts with label headbleed. Show all posts
Friday, January 30, 2009
Friday, November 28, 2008
Treat the patient, not the x-ray
Carolyn and I spoke with a pediatric neurosurgeon at Children's today who warned us that certain types of docs would scare the crap out of us when discussing Max's hydrocephalus. I've temporarily forgotten which of his fellow professionals he slandered, but I'm sure Cj will remind me. This guy said his maxim was "treat the patient, not the x-ray". He said that some kids just very obviously have problems from a very early age. Aside from terrifying constipation, Max appears to be a hardy young man. Indeed, he is extremely cute and engaging. On this basis, I choose not to worry too much.
Evening Update (Friday 11/28) -- Not a bad day at all
We spent the day at the NICU, and we also spoke with docs at Children's. In sum, not a terrible day at all. In fact, almost a good day.
On the northern front, we met with the attending for the day, who told us that he wasn't shocked by Max's head circumference growth. He also said it's not unusual to get a reduced volume of fluid via the LP, and that some of the CSF leaks out through the puncture anyway. He characterized the situation as a "holding pattern" while we wait to see if Max's body can learn to properly absorb CSF on its own. If Max's body doesn't, Max will need a shunt. But Max's doc doesn't expect any kind of emergent need to tap Max's ventricles in hurry. He's happy to wait a week or two to see what happens.
Max's attending also told us, and perhaps I misheard because I'm optimistic, that, at the moment, the hydrocephalus per se wasn't doing Max any damage. Any damage would have happened within a day or two of birth, but might not become visible until now as the body cleaned up waste, dead blood cells etc and the resulting holes in the white matter were uncovered. Is this bad news or good? It's a dilemma that has divided frequentists and Bayesians for a long time. But the midnight thought that somehow Max is suffering damage right now turns out to be wrong, and that's oddly comforting.
On the southern front, my personal diagnosis is that Max has scary constipation. His bowels don't move, gas builds up, his belly swells and the night staff freak out and quit feeding him. During the day today he got most of one feeding before spitting some of it back up and all of another while Carolyn held him. The high-tech medical team will convene again shortly to decide if it's appropriate to hit Max with the strongest medicine in their arsenal...prune juice. I'm not kidding. Well, he's too young to eat an unripe green apple, which always does the trick for me.
More on our conversations with docs at other hospitals later.
But on balance Carolyn and I feel much, much better this evening than we did this morning.
On the northern front, we met with the attending for the day, who told us that he wasn't shocked by Max's head circumference growth. He also said it's not unusual to get a reduced volume of fluid via the LP, and that some of the CSF leaks out through the puncture anyway. He characterized the situation as a "holding pattern" while we wait to see if Max's body can learn to properly absorb CSF on its own. If Max's body doesn't, Max will need a shunt. But Max's doc doesn't expect any kind of emergent need to tap Max's ventricles in hurry. He's happy to wait a week or two to see what happens.
Max's attending also told us, and perhaps I misheard because I'm optimistic, that, at the moment, the hydrocephalus per se wasn't doing Max any damage. Any damage would have happened within a day or two of birth, but might not become visible until now as the body cleaned up waste, dead blood cells etc and the resulting holes in the white matter were uncovered. Is this bad news or good? It's a dilemma that has divided frequentists and Bayesians for a long time. But the midnight thought that somehow Max is suffering damage right now turns out to be wrong, and that's oddly comforting.
On the southern front, my personal diagnosis is that Max has scary constipation. His bowels don't move, gas builds up, his belly swells and the night staff freak out and quit feeding him. During the day today he got most of one feeding before spitting some of it back up and all of another while Carolyn held him. The high-tech medical team will convene again shortly to decide if it's appropriate to hit Max with the strongest medicine in their arsenal...prune juice. I'm not kidding. Well, he's too young to eat an unripe green apple, which always does the trick for me.
More on our conversations with docs at other hospitals later.
But on balance Carolyn and I feel much, much better this evening than we did this morning.
Morning update (Friday 11/28): A lot of bad news
We've gotten a lot of bad news over the past 12 hours. Max's head circumference grew sharply yesterday afternoon; they tapped him again last night but only got 4 ccs of CSF. This suggests that, perhaps, his CSF is no longer communicating between the ventricles and the spine. And in the ensuing 8 hours his head circ grew again. No word yet on what the plan is.
His belly expanded enough to alarm everyone. They stopped his milk feeding and returned him to IV nutrition. They took an x-ray, presumably looking for signs of infection. That great medical authority, Dr. Google, indicates that people with cerebral palsy often have problems with their digestive systems. Who knows what's going on?
Finally, Max continues to retain fluid and appear somewhat swollen, despite efforts to change his diet, reduce is sodium and increase the protein content of his feeds.
His belly expanded enough to alarm everyone. They stopped his milk feeding and returned him to IV nutrition. They took an x-ray, presumably looking for signs of infection. That great medical authority, Dr. Google, indicates that people with cerebral palsy often have problems with their digestive systems. Who knows what's going on?
Finally, Max continues to retain fluid and appear somewhat swollen, despite efforts to change his diet, reduce is sodium and increase the protein content of his feeds.
Wednesday, November 26, 2008
Head bleeds, by the numbers
The docs measure head bleeds on quantitative scales. I'll try to update what we know about Max's head bleeds and associated hydrocephalus (aka the northern front). This may be disturbing, so feel free to skip the rest of this post. Max's head bleeds aren't the most important thing about him.
Our understanding is that Max had a grade 1 or 2 bleed on right side; this is not considered that serious and is generally thought to just be a risk factor for developmental delays. More seriously, Max also has a grade 3 bleed on the left side of his brain. This bleed is "periventricular", meaning that it is mostly inside the ventricle but that it had also involved the surrounding brain tissue. The MRI indicated that the extraventricular bleeding was, it seems, confined to the so-called "white matter" of the brain.
Our understanding is that Max had a grade 1 or 2 bleed on right side; this is not considered that serious and is generally thought to just be a risk factor for developmental delays. More seriously, Max also has a grade 3 bleed on the left side of his brain. This bleed is "periventricular", meaning that it is mostly inside the ventricle but that it had also involved the surrounding brain tissue. The MRI indicated that the extraventricular bleeding was, it seems, confined to the so-called "white matter" of the brain.
Learning about stressed-out preemies
Max had a big day today (barium study and a scheduled LP later today) so I didn't get him out of his crib. I did have a long conversation with one of his physical therapists about signs of stress in preemie infants. It turns out that there's a subtle but important distinction between preemies who are snuggling and those who are "shutting down" (a severe reaction to stress). Among the signs that your kid is shutting down: color change, grimacing, and As and Bs. All this time I thought he was just smiling at me!
We spoke to the doc who examined his barium study: no problems, and almost certainly not Hirschsprung's Disease. The slow bowel action was attributed, at worst, to his hydrocephalus. At best, it's just normal baby rhythm. The surgeon we spoke with asked about Max's head bleeds and hydrocephalus. He seemed really sad about them; I think we've made our peace with the likely consequences.
As for the incipient fluid-retention crisis, Max's sodium level was high and his protein level was low, so the kidneys were having trouble producing sufficient urine. One of Max's doctors kept talking about his BUN level. All I know about BUN I learnt from classic novel by Samuel Shem, The House of God, where Shem promulgates the nonsense law that BUN + Age = lasix dose. But I couldn't remember it and so missed my chance to impress his doctors. Oh well. Anyway, Max's age is like -0.2 years and they didn't give him lasix. The upshot is that they'll back off the supplemental sodium, increase his supplemental protein and expect his urine production to increase.
On the northern front, a head ultrasound showed a slight increase in ventricular volume, so his doctors will tap him later tonight. They will go for the standard 10 cc draw; earlier rumors of a bigger draw were simply baseless rumors.
We spoke to the doc who examined his barium study: no problems, and almost certainly not Hirschsprung's Disease. The slow bowel action was attributed, at worst, to his hydrocephalus. At best, it's just normal baby rhythm. The surgeon we spoke with asked about Max's head bleeds and hydrocephalus. He seemed really sad about them; I think we've made our peace with the likely consequences.
As for the incipient fluid-retention crisis, Max's sodium level was high and his protein level was low, so the kidneys were having trouble producing sufficient urine. One of Max's doctors kept talking about his BUN level. All I know about BUN I learnt from classic novel by Samuel Shem, The House of God, where Shem promulgates the nonsense law that BUN + Age = lasix dose. But I couldn't remember it and so missed my chance to impress his doctors. Oh well. Anyway, Max's age is like -0.2 years and they didn't give him lasix. The upshot is that they'll back off the supplemental sodium, increase his supplemental protein and expect his urine production to increase.
On the northern front, a head ultrasound showed a slight increase in ventricular volume, so his doctors will tap him later tonight. They will go for the standard 10 cc draw; earlier rumors of a bigger draw were simply baseless rumors.
Monday, November 24, 2008
Early thoughts on Max and his hydrocephalus
As described earlier, Max has a condition common to premature infants: hydrocephalus resulting from bleeding into his ventricles. He'll most likely have to have a shunt to control the pressure in his brain. If the Internet is to be believed, something like one million Americans have hydrocephalus and many of them have some form of shunt. In other words, casual empiricism suggests that hundreds of thousands of people are walking around this country with shunts in their brains.
Although we've only started investigating the condition, again, evidence from the Internet suggests that kids with hydrocephalus at birth have a variety of outcomes. Some have fairly significant cognitive and physical problems. Others appear unaffected. We don't yet know the frequency distribution across these outcomes.
As parents, we naturally want Max to have all the brainpower and physical abilities required for him to achieve his own hopes and dreams. We'll be gathering more information about the range of outcomes Max can expect, and how factors, such as physical and occupation therapy, that are under our control, can influence these outcomes.
We already know, however, the most important fact determining Max's future. He is our son.
Although we've only started investigating the condition, again, evidence from the Internet suggests that kids with hydrocephalus at birth have a variety of outcomes. Some have fairly significant cognitive and physical problems. Others appear unaffected. We don't yet know the frequency distribution across these outcomes.
As parents, we naturally want Max to have all the brainpower and physical abilities required for him to achieve his own hopes and dreams. We'll be gathering more information about the range of outcomes Max can expect, and how factors, such as physical and occupation therapy, that are under our control, can influence these outcomes.
We already know, however, the most important fact determining Max's future. He is our son.
Midday update (Monday 11/24)
Carolyn went in this morning to hold Max and to monitor medical developments. In addition, a nice man from Georgetown's building services retrieved her keys from the elevator well where they'd fallen last night. Also, Max has passed the 30 day mark, entitling Carolyn and me to free parking in the Georgetown garage. I'll report back on whether we get to use the card-only entrances and exits.
Max currently has two major medical issues: the head bleeds and the gut problems. We'll write more detailed descriptions of each problem, but you might find our earlier description of the Great NEC Scare useful background for Max's gut problems.
On the head bleed front, Max's head circumference grew over the weekend to just about where it was before Saturday's lumbar puncture (aka "tap"). Haifa tapped Max again around 11:30 AM and got about 10 ccs of CSF. The doctors report that Max's spinal area is becoming more fibrous and difficult to puncture. At today's tap, Haifa was able to get in with one stick, but had to move the needle around a little to get fluid. Rather than tap through an increasingly thick mass of fibers, Max's doctors are strongly considering installing a reservoir, which seems to be a kind of permanent tap through the skin of the head. More on this as it develops.
On the gut front (which we can't resist calling the "southern front"), Max pooped last night after Becky gave him a suppository. Max is scheduled for a barium enema study to help determine whether or not he has Hirschsprung's Disease (see The Great NEC Scare for more detail on Hirschsprung's). One of the surgeons dropped by Max's bedside and told Carolyn that he no longer thinks Max has Hirschsprung's, but this is based on, and I quote, "a hunch". The definitive test for Hirschsprung's involves a biopsy of the intestine, something we're eager to avoid. If the southern front problems aren't caused by Hirschsprung's or NEC, what are they caused by? What are the leading candidates? That's a great question, and I look forward to the answers.
In other news, physical therapist Anna dropped by Max's bedside. Max has a big day scheduled (LP plus barium enema) so he won't get physical therapy today. However, Anna did say that when she examined Max on Friday he was gestationally appropriate. Let me translate from medico-jargon: Max was bright-eyed, curious, looking around, waving his arms and legs around and doing all the other things that preemies of his age should be doing. This is good news, tempered only by the fact that, at this age, preemies shouldn't be doing a lot. Nonetheless, if there's one thing I can confidently say about Georgetown's NICU, it's that they never succumb to the soft bigotry of low expectations when it comes to their patients. It's hard work being a preemie in that place; they don't coddle those kids.
Max currently has two major medical issues: the head bleeds and the gut problems. We'll write more detailed descriptions of each problem, but you might find our earlier description of the Great NEC Scare useful background for Max's gut problems.
On the head bleed front, Max's head circumference grew over the weekend to just about where it was before Saturday's lumbar puncture (aka "tap"). Haifa tapped Max again around 11:30 AM and got about 10 ccs of CSF. The doctors report that Max's spinal area is becoming more fibrous and difficult to puncture. At today's tap, Haifa was able to get in with one stick, but had to move the needle around a little to get fluid. Rather than tap through an increasingly thick mass of fibers, Max's doctors are strongly considering installing a reservoir, which seems to be a kind of permanent tap through the skin of the head. More on this as it develops.
On the gut front (which we can't resist calling the "southern front"), Max pooped last night after Becky gave him a suppository. Max is scheduled for a barium enema study to help determine whether or not he has Hirschsprung's Disease (see The Great NEC Scare for more detail on Hirschsprung's). One of the surgeons dropped by Max's bedside and told Carolyn that he no longer thinks Max has Hirschsprung's, but this is based on, and I quote, "a hunch". The definitive test for Hirschsprung's involves a biopsy of the intestine, something we're eager to avoid. If the southern front problems aren't caused by Hirschsprung's or NEC, what are they caused by? What are the leading candidates? That's a great question, and I look forward to the answers.
In other news, physical therapist Anna dropped by Max's bedside. Max has a big day scheduled (LP plus barium enema) so he won't get physical therapy today. However, Anna did say that when she examined Max on Friday he was gestationally appropriate. Let me translate from medico-jargon: Max was bright-eyed, curious, looking around, waving his arms and legs around and doing all the other things that preemies of his age should be doing. This is good news, tempered only by the fact that, at this age, preemies shouldn't be doing a lot. Nonetheless, if there's one thing I can confidently say about Georgetown's NICU, it's that they never succumb to the soft bigotry of low expectations when it comes to their patients. It's hard work being a preemie in that place; they don't coddle those kids.
Subscribe to:
Comments (Atom)