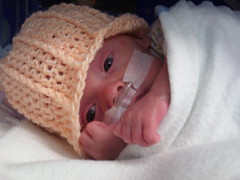
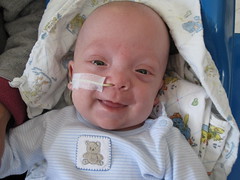
The NICU was roaring along at maximum capacity today, with temporary nurse R. again being called in to take care of Max. He's a floater from another service in the hospital, and Carolyn and I really like him. From what Carolyn can see through the windows, the higher-level NICU appears to be more hectic than usual.
Carolyn bottle fed Max twice today, once at his noon feed and again at his 3:00 PM feed. He took 12 ccs at noon but it was otherwise unremarkable. However, speech therapist S. dropped by and observed Carolyn's afternoon feeding. S. was extremely positive: Max's coordination was good, he was pausing appropriately, and was trying to grasp the bottle. S. said that Max's breathing was excellent: "I hesitate to use the word 'strong' with respect to Max". After a while Max seemed to get tired, and he demurred when Carolyn offered him the bottle once, then did so again when offered the bottle a second time, but Max took the bottle on the third offer. He swallowed a mouthful of formula and then spat it back up. He choked on it and had a brady--his heart rate dropped to 80 beats/minute. Max recovered on his own: this episode was nothing close to a dreaded ALTE. S. was totally unfazed and showed Carolyn how to avoid future choking episodes in similar situations (it's a matter of geometry--Carolyn showed me using a large frog puppet here at home).
Dr. R., the NICU attending, after discussing the matter with Carolyn, has put Max back on pediatric neurosurgery rounds. This means that Max will be seen by a fellow or attending routinely until they again sign off on him, as they did earlier this year. The peds neuro service will likely order a CT and/or MRI to evaluate Max for shunt placement. Their snap judgment remains that he is a "borderline" case.
Carolyn and Dr. R. had a long and involved conversation about the potential future courses that Max's treatment could take. It's exactly the kind of conversation we've been having often, and it's draining in a way that's hard to communicate. Carolyn or I, and the physician, try to understand the various contingencies that might crop up in Max's increasingly complex care. Max could need a shunt fairly soon. But he could need a Nissen soon, and then need a shunt. Or he might get strong enough to go the HSC, then need a shunt and then need a Nissen. Ideally, the shunt would empty into Max's intestinal space, but if his GI system was upset, it might temporarily be drained from his head. And on and on and on. These conversations usually peter out with less-than-conclusive statements such as "we'll have to wait and see" or "the next move is up to Max." Dr. R., however, concluded the conversation by saying "My goal is to get Max home."
skip to main |
skip to sidebar

Max was born in October 2008 at Georgetown University Hospital. After more than four months at GUH, Max moved to the HSC Pediatric Center in March 2009. He came home six months after he was born, in April 2009.
A TUBE-FREE MORNING

Start Here: A list of posts with background information
- We're home! (leaving the hospital with Max)
- The hospital at home (what it's like to care for Max at home)
- Max in action (see Max do his tricks)
- How is Max? (update April 2009)
Most recent photos of Max
Blog Archive
-
▼
2009
(224)
-
▼
February
(41)
- Evening update (Saturday 2/28)
- Evening Update (Friday 2/27)
- Out for a stroll
- Evening update (Thursday 2/26)
- Proposed feeding schedule
- Evening update (Wednesday 2/25)
- Evening update (Tuesday 2/24)
- Evening update (Monday 2/23)
- Evening Update (Sunday 2/22)
- Sunday in the NICU
- Evening Update (Saturday 2/21)
- Evening update (Friday 2/20)
- Evening Update (Thursday 2/19)
- Assessment by the peds neuro service
- Max relaxing in the new crib
- Max's new digs
- Evening Update (Wednesday 2/18)
- Evening Update (Tuesday 2/17)
- Evening Update (Monday 2/16)
- Evening Update (2/15)
- Late night update (Saturday 2/14)
- Max and the soothie
- Evening update (Saturday 2/14)
- Gorilla nursery
- Morning update (Monday 2/14)
- Evening Update (Friday 2/13)
- Treating the baby, not the x-ray (part 2)
- Evening Update (Thursday 2/12)
- Evening update (Wednesday, 2/11)
- Max's next stop
- Max's second report card
- Evening update (Sunday 2/8)
- Evening Update (Saturday 2/7)
- Evening Update (Friday 2/6)
- Evening Update (Thursday 2/5)
- A day at the NICU
- Holding paws with Max
- Evening Update (Tuesday 2/3)
- Evening Update (Monday 2/2)
- Late night update (Sunday 2/1)
- Evening Update (Sunday 2/1)
-
▼
February
(41)